Yes, acute kidney injury can often be cured or reversed with prompt treatment, and many patients recover full kidney function, though the recovery timeline and extent vary based on the cause and severity of injury.
What is Acute Kidney Injury Recovery?
Acute kidney injury is fundamentally different from chronic kidney disease in one critical aspect—reversibility. Unlike chronic kidney disease, which involves permanent, progressive damage, AKI represents a sudden decline in kidney function that can often be reversed when the underlying cause is identified and treated promptly.
Treatment for acute kidney injury most often means a hospital stay, and how long patients stay depends on the reason for their acute kidney injury and how quickly their kidneys recover. The key to successful treatment lies in finding and addressing the illness or injury that damaged the kidneys.
Research published in various medical journals indicates that with proper medical care, many patients recover normal kidney function. However, the prognosis varies depending on the severity of kidney damage and the promptness of treatment. Some patients may develop chronic kidney disease as a complication, which is why early intervention is crucial.
What Does Treatment for Acute Kidney Injury Involve?
Treatment for AKI is primarily supportive in nature and focuses on treating the underlying cause while preventing complications. The current approach involves managing the condition while giving the kidneys time to heal naturally.
Identifying and treating the underlying cause is the first priority. This might involve stopping medications that are damaging the kidneys, treating infections with antibiotics, removing urinary blockages, or managing conditions like heart failure or liver disease.
Fluid and electrolyte management forms a cornerstone of AKI treatment. If dehydration caused the kidney injury, patients may need intravenous fluids to restore blood flow to the kidneys. Conversely, if AKI causes fluid accumulation leading to swelling in the arms and legs, diuretics may be prescribed to help the body eliminate extra fluids.
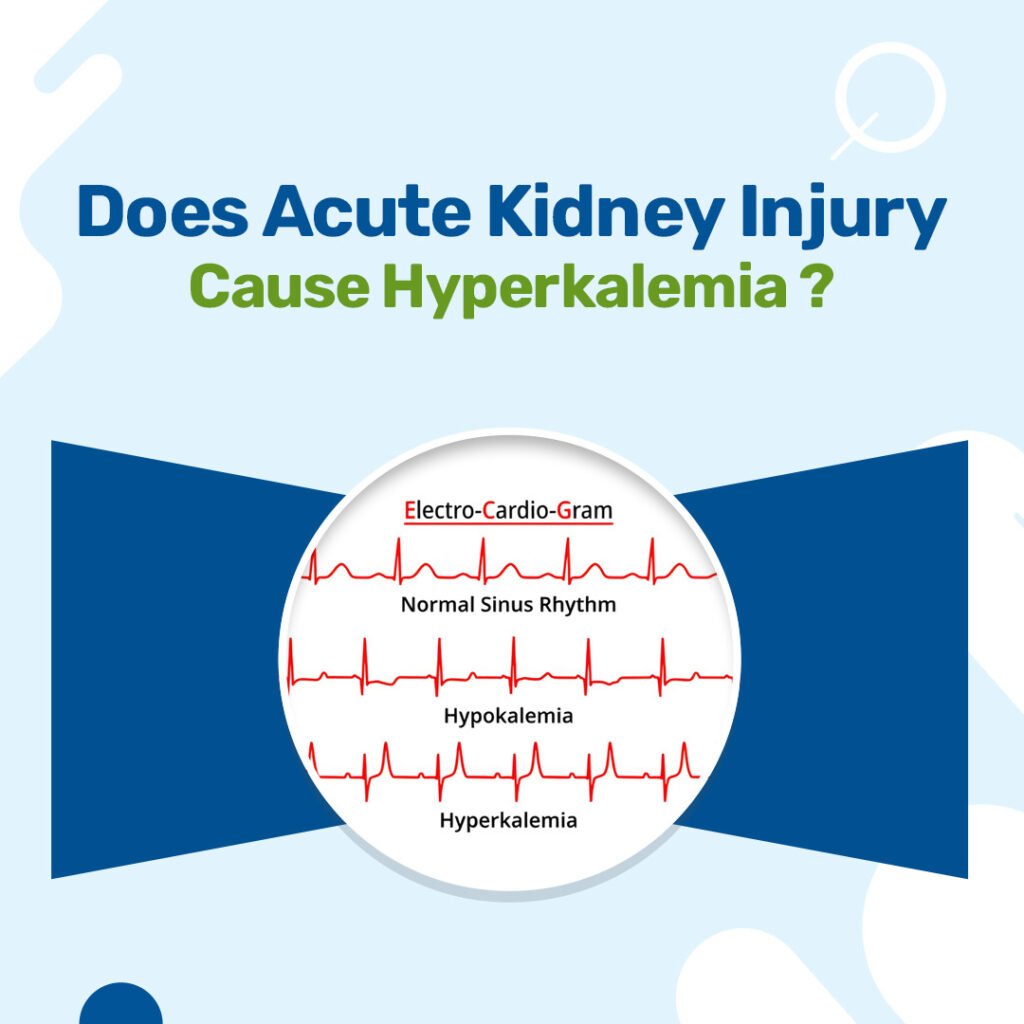
Electrolyte balance requires careful monitoring and correction. The kidneys might not filter potassium adequately, so medicines called potassium binders may be necessary to prevent dangerous buildups that can cause irregular heartbeats and muscle weakness. Similarly, if calcium levels drop too low, calcium infusions may be required.
Dialysis may be necessary in severe cases. When waste products build up in the blood to dangerous levels, hemodialysis can remove toxins and excess fluids while the kidneys heal. According to the National Kidney Foundation, in most cases, dialysis treatments are only temporary until the kidneys can recover. Dialysis is considered when symptoms like severe electrolyte imbalances, uremia, or fluid overload pose life-threatening risks.
Medication adjustments are essential during AKI treatment. Nephrologists carefully review all medications to avoid further kidney damage, discontinuing or replacing drugs that are toxic to the kidneys such as NSAIDs and certain antibiotics. Blood pressure medications, infection treatments, and therapies for complications like metabolic acidosis are prescribed as needed.
Can All Patients with AKI Recover Completely?
While many patients with AKI achieve complete recovery, outcomes vary significantly. The prognosis depends on several factors including the severity and underlying cause of the kidney injury, the patient’s overall health, and how quickly treatment begins.
According to research, with prompt treatment, many patients recover fully. However, even after treatment, some people may not fully recover kidney function. AKI can increase the risk for chronic kidney disease or make existing CKD worse.
The American Kidney Fund reports that after having AKI, patients have a higher risk for other health problems such as chronic kidney disease, heart disease, or stroke, and are also at higher risk of getting AKI again in the future. This makes regular follow-up visits with healthcare professionals essential, starting ideally within three months of finishing treatment.
Studies show that the severity of AKI significantly impacts recovery potential. Patients with mild AKI who receive prompt treatment have excellent chances of complete recovery, while those with severe AKI requiring prolonged dialysis may face a higher risk of residual kidney impairment.
What Factors Influence Recovery from AKI?
Several key factors determine whether a patient will achieve complete recovery from acute kidney injury.
Timeliness of diagnosis and treatment is perhaps the most critical factor. Early recognition of AKI symptoms and immediate medical intervention significantly improve outcomes. Delays in treatment can lead to more extensive kidney damage and reduce the likelihood of full recovery.
Underlying cause and reversibility play a crucial role. Prerenal AKI caused by dehydration or temporary reduction in blood flow typically has better recovery rates compared to intrinsic renal AKI involving direct kidney tissue damage. Postrenal AKI from urinary obstruction often resolves completely once the blockage is removed.
Severity of kidney damage impacts recovery potential. Mild AKI with modest elevations in creatinine levels generally has better prognosis than severe AKI requiring dialysis. The duration of kidney dysfunction also matters—prolonged AKI increases the risk of permanent damage.
Patient’s overall health status influences recovery. Patients with pre-existing chronic conditions like diabetes, hypertension, or heart disease may face more challenging recovery paths. Age and nutritional status also affect healing capacity.
Prevention of complications during the acute phase is essential. Effective management of fluid balance, electrolyte disturbances, and metabolic acidosis while the kidneys heal can prevent secondary damage.
How Long Does Recovery from AKI Take?
The recovery timeline for acute kidney injury varies considerably among patients. How long patients stay in the hospital depends on the reason for their acute kidney injury and how quickly their kidneys recover.
For mild cases of AKI treated promptly, kidney function may begin improving within days to weeks. Patients with prerenal AKI often show rapid improvement once adequate hydration and blood flow are restored. However, more severe cases, particularly those involving direct kidney tissue damage, may require weeks to months for recovery.
During recovery, kidney function is monitored through regular blood tests measuring creatinine and blood urea nitrogen levels. Urine output is also tracked as an indicator of improving kidney function. In cases requiring dialysis, the need for renal replacement therapy gradually decreases as native kidney function returns.
Even after hospital discharge, continued monitoring is essential. The National Kidney Foundation recommends regular follow-up visits to check kidney health, ideally starting within three months of completing AKI treatment. These appointments help detect any developing complications early and adjust treatment plans as needed.
What Can Patients Do to Support Recovery?
Patient participation in recovery is crucial for optimal outcomes. Following medical advice and making appropriate lifestyle modifications can significantly enhance healing.
Dietary modifications support kidney recovery. Doctors may refer patients to a registered dietitian who can develop a kidney-friendly eating plan. This typically involves managing protein intake, limiting sodium, controlling potassium and phosphorus levels, and ensuring adequate calorie consumption.
Hydration management requires careful attention. While staying hydrated is generally important for kidney health, patients recovering from AKI need individualized guidance based on their specific situation. Some may need increased fluid intake, while others with fluid retention may need restrictions.
Medication compliance is essential. Patients must take prescribed medications as directed and avoid nephrotoxic drugs without consulting healthcare providers. Over-the-counter medications like NSAIDs should be avoided or used only under medical supervision.
Managing chronic conditions helps prevent recurrent AKI. Controlling blood pressure, managing diabetes, and treating any underlying conditions reduces the risk of future kidney injury. Regular check-ups with healthcare providers allow for monitoring and adjustments to treatment plans.
Lifestyle modifications promote overall health and kidney function. This includes maintaining a balanced diet, engaging in appropriate physical activity as recommended by healthcare providers, avoiding smoking, and limiting alcohol consumption.
Can AKI Be Prevented?
While it can be challenging to predict or prevent all cases of acute kidney injury, certain measures can reduce risk. A healthy lifestyle and taking good care of the kidneys can help protect against AKI.
Staying hydrated is one of the most effective preventive measures, particularly during illness, hot weather, or increased physical activity. Adequate hydration helps maintain blood flow to the kidneys and supports their filtering function.
Avoiding nephrotoxic medications when possible protects kidney health. Patients should inform all healthcare providers about their kidney function and ask about the kidney safety of prescribed medications. Those with risk factors for AKI should be especially cautious with NSAIDs, certain antibiotics, and contrast dyes used in imaging studies.
Managing chronic conditions effectively reduces AKI risk. Controlling high blood pressure and diabetes through medication, diet, and lifestyle modifications protects kidney function. Regular monitoring of these conditions allows for early intervention if problems develop.
Seeking prompt medical attention for infections, urinary problems, or other health concerns can prevent conditions from progressing to AKI. Early treatment of infections, prompt relief of urinary obstructions, and timely management of dehydration can protect the kidneys.
Regular kidney function monitoring for high-risk individuals enables early detection of problems. Those with diabetes, hypertension, heart disease, or previous episodes of AKI should have their kidney function checked regularly.
Can Kidney Disease Cause Hand Tremors?
Kidney disease causes hand tremors. Involuntary movements like tremor, myoclonus, and asterixis occur with chronic kidney disease (CKD) and renal dysfunction. End-stage renal disease presents with various nonspecific signs. Azotemia and electrolyte abnormalities contribute to movement disorders. Asterixis, or “flapping tremor,” frequently arises from toxic metabolic encephalopathy due to renal or hepatic disorders. Kidney failure results in tremor and muscle and nerve damage.
Does Acute Kidney Disease Go Away?
Acute kidney injury (AKI) goes away for most people. Kidney damage reverses with prompt treatment of acute kidney failure. Treatment includes identifying the cause and preventing further damage. Most people with AKI make a full recovery. Early treatment prevents lasting kidney damage. Untreated, severe AKI proves fatal. A small number of patients develop chronic kidney disease or long-term kidney failure.
How Can Acute Kidney Injury Be Prevented?
Acute kidney injury (AKI) prevention includes maintaining hydration and managing chronic health conditions. Patients maintain adequate mean arterial pressure above $65 \text{ mmHg}$ and avoid fluid overload. Prevention involves treating bad infections quickly. People avoid nephrotoxic drugs when possible. Strategies include monitoring serum drug levels and renal function. Increasing fluid intake during a fever or on hot days helps prevent AKI.
Conclusion
Acute kidney injury can often be cured or reversed with prompt, appropriate treatment, though recovery outcomes vary based on the severity of injury, underlying cause, and timeliness of intervention. Unlike chronic kidney disease, AKI represents a potentially reversible condition when the kidneys are given time to heal while receiving proper supportive care.
The key to successful recovery lies in early recognition of symptoms, immediate medical attention, identification and treatment of the underlying cause, and comprehensive supportive care. While many patients achieve complete recovery of kidney function, some may develop chronic kidney disease or remain at increased risk for future kidney problems, making long-term follow-up essential.
If you or a loved one is dealing with acute kidney injury or has risk factors for kidney disease, expert nephrology care is crucial for optimal outcomes. Dr. Vishal Golay is a leading nephrologist in Siliguri with over 15 years of experience in diagnosing and treating kidney diseases. With a patient-centric approach and evidence-based practice, Dr. Golay offers comprehensive kidney care services including acute kidney injury treatment, dialysis support, chronic kidney disease management, and personalized follow-up care to prevent complications.


 7430923244
7430923244