Patients ask this question many times in clinic: is chronic kidney disease (CKD) directly caused by alcohol? The short answer is that alcohol can harm kidneys through several pathways—especially at heavy levels or in the presence of other conditions like high blood pressure and liver disease but evidence from large cohort studies and meta-analyses is mixed on whether alcohol itself directly “causes” CKD. Some research even suggests that light-to-moderate intake is associated with a lower incidence of CKD, while heavy drinking can worsen kidney-related risk factors such as hypertension and albuminuria.

What Research Says at a Glance
- Experimental and mechanistic studies show alcohol can induce oxidative stress, inflammation, and direct tubular injury in kidneys, independent of liver damage.
- Observational cohorts and meta-analyses report mixed results: several find light-to-moderate drinking associated with lower CKD incidence, while heavy drinking links to higher albuminuria and clinical risks that threaten kidneys.
- Kidney health organizations advise limiting alcohol because it can raise blood pressure, dehydrate, and complicate kidney disease management—particularly in those already living with CKD.
How Alcohol Affects The Kidneys Biologically?
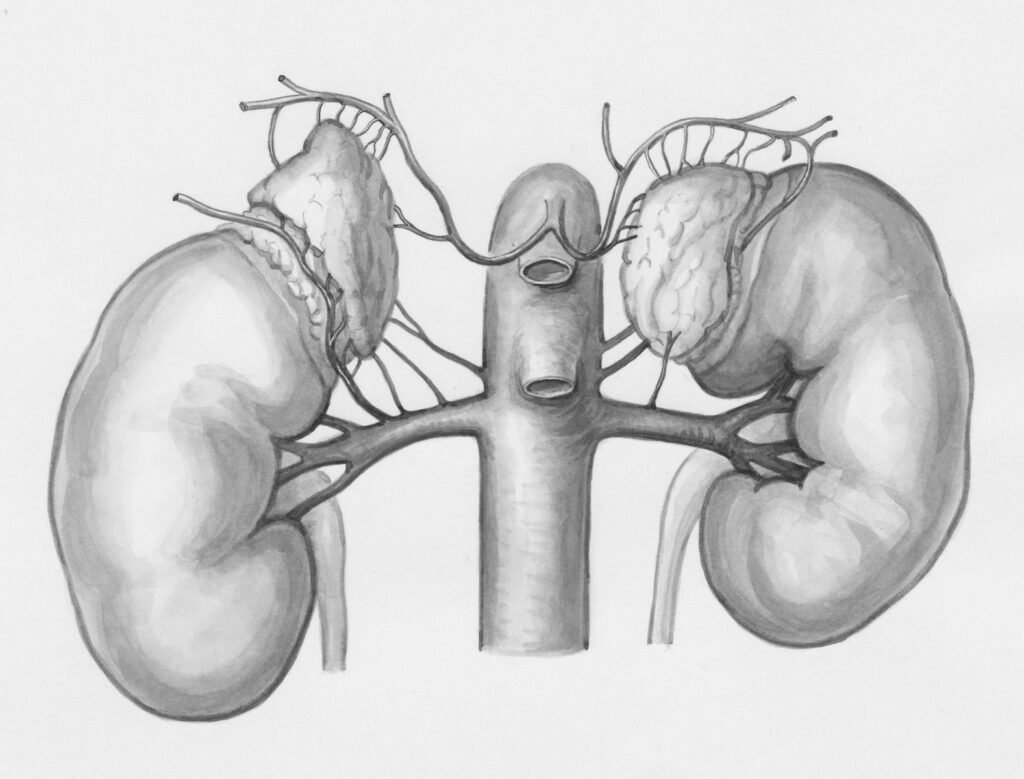
Alcohol is mostly metabolized in the liver, but the kidneys also contribute to metabolism and excretion; around 10% of ingested ethanol is excreted unchanged in urine. Enzymes such as alcohol dehydrogenase and CYP2E1 are present in renal tissue, and excessive intake can generate reactive oxygen and nitrogen species, driving oxidative stress, microvascular/hemodynamic changes, and inflammation within the kidneys. Animal models demonstrate leukocyte infiltration and structural kidney damage after prolonged ethanol exposure, indicating potential direct renal injury beyond liver-related effects.
These mechanisms explain why heavy or prolonged alcohol use may impair renal function, aggravate blood pressure, dysregulate fluids/electrolytes, and interact adversely with medications—all of which increase CKD risk or accelerate progression.
Epidemiology: does alcohol increase or decrease CKD risk?
Evidence is nuanced and depends on the amount of alcohol consumed, population studied, and outcomes measured.
- Meta-analysis of 15 prospective cohorts (268,723 participants) found that low to moderate intake (<60 g/day) was associated with a lower risk of chronic kidney damage (including declined GFR and proteinuria) compared with non/occasional drinkers; severe intake (≥60 g/day) did not show benefit and suggested a nonsignificant increase in risk.
- A meta-analysis of 20 studies reported an inverse association between high alcohol consumption and CKD in men (pooled RR ~0.72), with no significant association for proteinuria or end-stage renal disease overall; this highlights sex differences and heterogeneous definitions of “high” intake across studies.
- An Australian 5-year cohort observed that intake ≥30 g/day correlated with increased albuminuria risk after adjustment—an early sign of kidney damage—even as some other cohorts reported lower CKD incidence with moderate drinking.
- A large Taiwanese cohort (45,200 adults; 8.5 years follow-up) found social and regular drinkers had a lower incidence of new-onset CKD than non-drinkers after adjusting for confounders, illustrating potential protective associations at modest levels.
Interpreting these findings requires caution. Observational studies can be confounded by lifestyle and health differences between abstainers and moderate drinkers (e.g., the “sick quitter” effect). Definitions of “moderate” vary across studies, and endpoints (eGFR decline vs. albuminuria vs. ESRD) differ. Nonetheless, across multiple cohorts and meta-analyses, consistent patterns emerge: light-to-moderate drinking is often associated with lower CKD incidence, while heavier patterns are linked to risks (hypertension, albuminuria) that can harm kidneys.
Practical implications for people with or at risk of CKD
- Blood pressure and hydration: Alcohol raises blood pressure in a dose-dependent fashion and can cause dehydration—both harmful to kidney health.
- Medication interactions: Alcohol can interact with antihypertensives, diuretics, and diabetes medications, complicating CKD management.
- Underlying liver disease: Alcohol-related liver disease can secondarily impair renal function (e.g., hepatorenal physiology), intensifying kidney risk.
- Existing CKD: Kidney organizations recommend limiting alcohol; individualized limits depend on stage of CKD, comorbidities, and medications.
In short, while modest intake may not directly cause CKD and can correlate with lower CKD incidence in some populations, it is not a “treatment,” and any level beyond modest—especially daily or heavy use—can harm kidney health through blood pressure elevation, albuminuria, dehydration, and metabolic stress.
How much is “light,” “moderate,” or “heavy”?
Research definitions vary. One meta-analysis categorized intake as low (<13 g/day), moderate (13–26 g/day), high (26–60 g/day), and severe (≥60 g/day). For context, 10–14 g of alcohol approximates one standard drink in many countries. Importantly, safe limits must be individualized—especially in CKD—taking into account eGFR, albuminuria, blood pressure, cardiovascular risk, diabetes control, and medications.
Who should avoid alcohol?
- Individuals with advanced CKD, uncontrolled hypertension, refractory edema, or recurrent dehydration.
- Those with alcohol use disorder, liver disease, pancreatitis, or frequent gout flares (beer and spirits can raise uric acid).
- Patients on interacting medications (e.g., sedatives, certain neuropathy treatments) or with poor diabetes control where hypoglycemia risk is heightened.
These groups face amplified kidney and systemic risks from alcohol, and abstinence or strict medical guidance is prudent.
Evidence-based takeaways
- Alcohol does not uniformly or inevitably “cause” CKD, but heavy and prolonged consumption can damage kidneys via oxidative stress, inflammation, hypertension, albuminuria, and fluid/electrolyte disturbances.
- Light-to-moderate intake is often associated with lower CKD incidence in cohorts and meta-analyses, especially among men, though causality is uncertain and benefits may reflect confounding lifestyle factors.
- For people living with CKD—or with risk factors like hypertension, diabetes, or liver disease—most guidelines prioritize limiting alcohol to protect kidney function, blood pressure, and medication safety.
What to discuss with a nephrologist
- Current kidney status: eGFR trend, albuminuria level, blood pressure readings.
- Full cardiovascular risk profile: diabetes control, lipid levels, BMI, smoking status.
- Actual drinking pattern: weekly units, binge episodes, hydration practices.
- Medication interactions: antihypertensives, diuretics, SGLT2 inhibitors, RAAS blockers, analgesics.
- Personalized limits: aligning alcohol advice with kidney function and comorbidities.
Conclusion and next steps with Dr. Vishal Golay
Alcohol’s relationship with CKD is nuanced: light-to-moderate drinking often correlates with lower CKD incidence in observational research, while heavy use drives mechanisms that harm kidneys and worsens clinical risk factors like hypertension and albuminuria. Anyone with existing CKD or cardiometabolic risks should approach alcohol cautiously and personalize decisions with their nephrologist.

For individualized guidance, book a consultation with Dr. Vishal Golay’s nephrology service in Siliguri for:
- A comprehensive kidney risk assessment (eGFR, urine albumin, blood pressure profile).
- A tailored alcohol and lifestyle plan aligned with current kidney function, medications, and goals.
- Ongoing monitoring to protect kidney health while addressing cardiovascular and metabolic risks.
Key sources mentioned:
- Fan Z et al., Alcohol Consumption Can be a “Double-Edged Sword” for Chronic Kidney Disease Patients.
- Li D et al., Alcohol Drinking and the Risk of Chronic Kidney Damage: Meta-Analysis of 15 Prospective Cohorts.
- Cheungpasitporn W et al., High alcohol consumption and the risk of renal damage: Meta-analysis.
- White SL et al., Alcohol consumption and 5-year onset of CKD (albuminuria risk at ≥30 g/day).
- National Kidney Foundation and American Kidney Fund guidance on alcohol and kidneys.
 7430923244
7430923244




