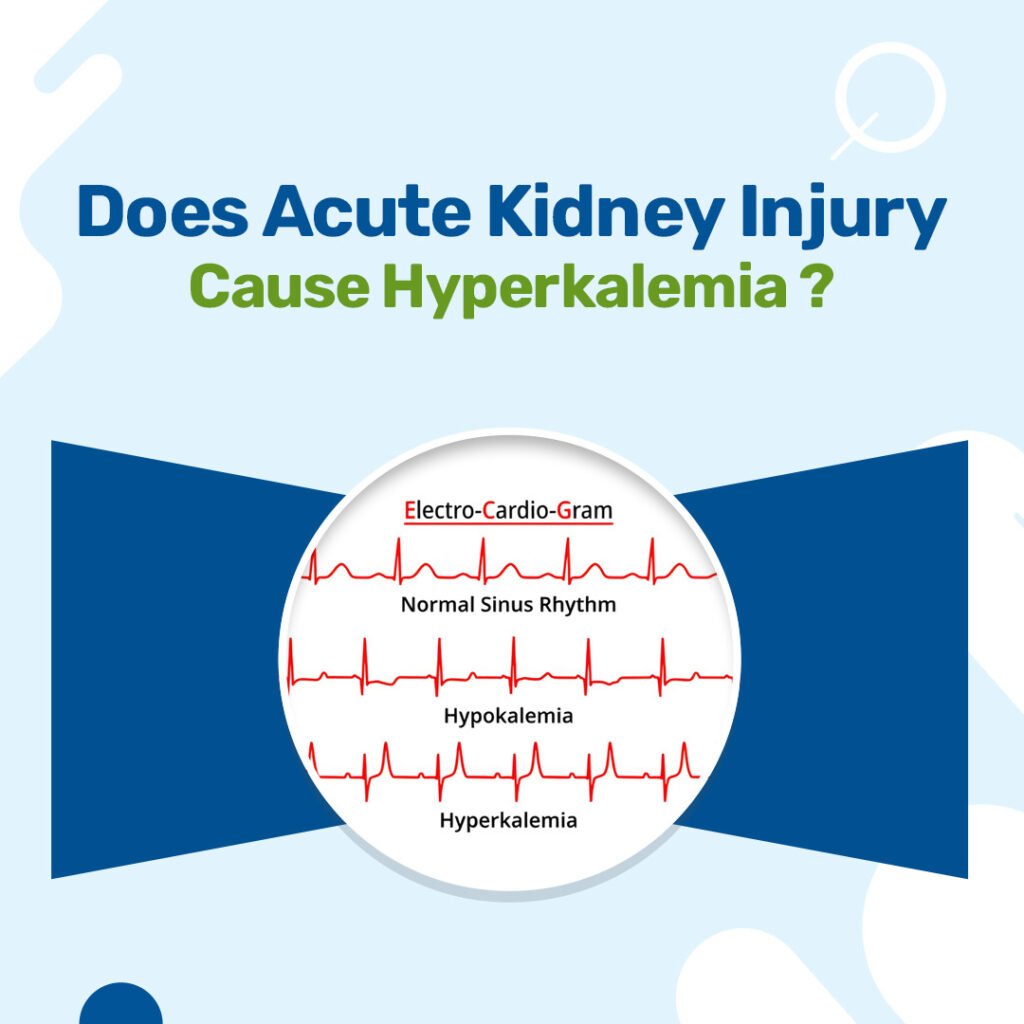
Chronic kidney disease (CKD) typically develops gradually over time from ongoing damage due to factors like diabetes or hypertension, rather than happening suddenly. While it progresses slowly through persistent stress on kidney filters, certain triggers such as dehydration or infections can worsen symptoms abruptly, mimicking a sudden onset. Distinguishing CKD from acute kidney injury (AKI), which strikes quickly and is often reversible with prompt care, is key to proper management.
Early signs include foamy urine, persistent fatigue, leg swelling, high blood pressure, and itchy skin, often caught via eGFR blood tests. High-risk groups, like those with diabetes or post-transplant patients, benefit from regular monitoring to prevent rapid decline.
Management involves lifestyle changes such as low-sodium diets, controlling blood pressure below 130/80, 150 minutes of weekly exercise, balanced hydration, and quitting smoking. These steps slow progression and reduce complications, supporting long-term kidney health.
Key Takeaways:
-
Chronic Kidney Disease (CKD) rarely develops suddenly; it’s typically a slow progression from causes like diabetes and hypertension, unlike acute kidney injury which strikes abruptly.
-
Triggers like infections or medications can accelerate CKD, making it seem sudden, but it builds over time—early detection is crucial to prevent rapid decline.
-
High-risk groups include those with diabetes, hypertension, or prior acute kidney injury; consult a nephrologist for personalized plans to slow progression.
Can Chronic Kidney Disease Develop Suddenly?
While Chronic Kidney Disease (CKD) is typically progressive, it is important to distinguish it from sudden-onset conditions like Acute Kidney Injury through expert diagnosis. CKD builds over time from ongoing damage, but certain triggers can worsen it quickly. This sets it apart from acute issues that demand different care.
CKD management focuses on long-term strategies like blood pressure control and lifestyle changes. In contrast, acute kidney injury treatment often involves immediate steps such as fluid balance and dialysis support. Evidence-based practice helps prevent misdiagnosis by using precise tests.
Patients sometimes confuse the two because symptoms like fatigue overlap. Early differentiation ensures the right path, avoiding unnecessary urgency or delays. Experts recommend regular check-ups for those at risk from diabetes or hypertension.
Understanding this difference answers the question: Can Chronic Kidney Disease happen suddenly? Not typically, yet swift expert evaluation clarifies any rapid changes. Tailored approaches support better outcomes.
Key Differences Between CKD and Acute Kidney Injury
CKD develops gradually from ongoing damage like hypertension-related disorders, while Acute Kidney Injury strikes suddenly and requires advanced diagnostic protocols. This distinction guides proper care and prevents confusion. Here’s a clear comparison.
| Condition |
Onset |
Common Causes |
Treatment Approach |
Prognosis |
| CKD |
Gradual |
Diabetes, hypertension |
Comprehensive management with medications and diet |
Slow progression with ongoing monitoring |
| AKI |
Sudden |
Dehydration, infection |
Hemodialysis support and cause-specific care |
Reversible with early intervention |
Consider these practical use cases. For CKD post-transplant follow-up, kidney function is monitored with routine blood tests and immunosuppressants are adjusted to manage gradual decline. Patients learn to track symptoms daily for steady control.
In AKI dialysis care, urgent dialysis restores balance after sudden dehydration from illness. Quick reversal through hydration and infection treatment is prioritized. Recovery often follows prompt action, highlighting the need for speed.
Why CKD Is Typically a Slow, Progressive Condition
CKD progresses slowly over years due to persistent factors like uncontrolled hypertension. This gradual damage builds from ongoing stress on kidney filters, or nephrons. Evidence-based practices for CKD management highlight how early detection can change this path.
Unlike sudden injuries, CKD develops quietly from repeated harm to kidney tissue. Factors like high blood pressure strain blood vessels over time. Patients often notice no symptoms until later stages, making regular check-ups key.
Early screening allows interventions that slow or halt progression. Healthcare providers focus on controlling root causes to preserve kidney function. This approach answers why many wonder, can chronic kidney disease happen suddenly, when it rarely does.
Monitoring and lifestyle adjustments help patients avoid advanced CKD. Consistent care transforms the typical slow decline into manageable health.
Common Gradual Causes Like Diabetes and Hypertension
Diabetes and hypertension are primary drivers of CKD’s slow damage to nephrons, often requiring specialized evaluation for hypertension-related kidney disorders. These conditions harm kidneys bit by bit over years. High glucose from diabetes and vessel strain from hypertension weaken filters steadily.
Here are four common gradual causes:
-
Hypertension damages kidney blood vessels, leading to scarring over time.
-
Diabetes causes high blood sugar to harm delicate filters, reducing function gradually.
-
Prolonged untreated issues like infections allow damage to build without notice.
-
Kidney stones contribute slowly by causing repeated blockages and inflammation.
Experts recommend yearly checks for blood pressure and glucose levels to catch issues early. Simple habits like a balanced diet support kidney health. These steps prevent the slow creep toward CKD.
Patients with these risks benefit from tailored plans. Regular monitoring spots changes before they worsen. This focus keeps CKD from advancing unnoticed.
Can Any Triggers Make CKD Seem Sudden?
Though gradual, CKD can appear sudden when advanced stages are unmonitored. This highlights the importance of early detection. Triggers like dehydration, medications, or infections can unmask hidden damage, making chronic kidney disease seem to happen suddenly.
Severe dehydration often exacerbates underlying CKD, linking it to acute kidney injury (AKI). Without enough fluids, kidneys struggle, revealing silent progression. Personalized hydration plans with lifestyle guidance can help prevent this.
Medication toxicity in undiagnosed cases can spike damage quickly. Common drugs strain kidneys if pre-existing issues are hidden. Medication reviews and dietary advice help reduce risk.
Infections accelerate kidney harm in vulnerable people. Acute kidney injury treatment prevents escalation to CKD, per KDIGO guidelines. A warning: 20% of AKI leads to CKD. Monitoring and prompt care are essential.
Sudden Dehydration and Hidden CKD
Dehydration triggers AKI on top of undetected CKD, causing a sudden drop in function. Patients may feel extreme fatigue or confusion quickly. Rehydration therapy reverses this, but early checks help stop escalation.
Track fluid intake daily and aim for consistent hydration through water-rich foods and routines. This plan spots risks before they worsen.
Examples include summer heat or illness causing fluid loss. Monitor urine color and volume. Lifestyle guidance focuses on prevention to avoid sudden CKD flares.
Medication Toxicity in Undiagnosed Cases
Certain painkillers or antibiotics build up in weakened kidneys, mimicking sudden CKD onset. Toxicity hits hard without prior monitoring. Drug level tests catch this early.
Review all medications regularly and consider kidney-friendly diets low in processed items. Adjustments help keep function stable.
Practical steps: List all supplements before new prescriptions. Regular blood work guides safe use. This approach prevents toxicity from unmasking hidden disease.
Infections Accelerating Kidney Damage
Urinary tract or systemic infections inflame kidneys, speeding CKD in at-risk cases. Symptoms like fever and swelling appear abruptly. Antibiotic protocols plus supportive care halt progression.
Infection prevention through hygiene and vaccines is important. Monitor for early signs with routine visits. Lifestyle tweaks can boost immunity.
Seek care at the first sign of fever in anyone with a CKD history. Hydrate extra during illness. These steps help ensure infections do not trigger sudden worsening.
How Does Acute Kidney Injury Relate to CKD Progression?
Repeated Acute Kidney Injury (AKI) episodes can accelerate CKD progression through the need for hemodialysis or peritoneal dialysis support. AKI causes a sudden drop in kidney function, often measured by glomerular filtration rate (GFR). This relates to chronic kidney disease because incomplete recovery from AKI can lead to lasting damage, answering whether chronic kidney disease can happen suddenly through repeated acute events.
AKI acts as a trigger for CKD in many cases. A single AKI event stresses the kidneys, and without full recovery, scar tissue forms. Over time, this sets the stage for progressive kidney decline.
-
AKI episode: Sudden GFR drop from dehydration, infection, or toxins disrupts kidney filtration.
-
Incomplete recovery: Kidneys scar, reducing long-term function even after the acute phase ends.
-
Repeated events: Multiple AKI incidents push kidneys into CKD stages, with declining GFR levels.
-
Dialysis intervention: Hemodialysis or peritoneal dialysis slows progression to Stage 3 CKD by supporting kidney rest and toxin removal.
Research suggests AKI survivors face higher CKD risk. Seek dialysis care post-AKI to monitor GFR and prevent advancement. Early intervention offers practical support through tailored dialysis plans.
What Are the Earliest Signs of CKD Onset?
Subtle early CKD signs like fatigue and swelling often go unnoticed, but expert diagnosis enables timely intervention. The earliest indicators of chronic kidney disease onset include foamy urine, persistent tiredness, leg swelling, high blood pressure, and itchy skin. Spotting these prompts quick checks like an eGFR blood test for confirmation.
These signs signal kidneys struggling to filter waste. Early detection through simple tests helps manage the condition before it worsens. Research suggests catching it early improves long-term kidney health.
-
Foamy urine points to proteinuria, where excess protein leaks into urine. This happens as kidney filters weaken. Get an eGFR blood test to measure filtration rate and confirm damage.
-
Persistent fatigue stems from anemia or toxin buildup. Kidneys fail to produce enough erythropoietin for red blood cells. An eGFR test assesses if this ties to early CKD.
-
Swelling in legs, or edema, occurs from fluid retention due to poor sodium balance. Check with an eGFR blood test alongside urine analysis for protein levels.
-
High blood pressure strains kidneys further, creating a cycle. Itchy skin results from mineral imbalances like high phosphorus. Both warrant an immediate eGFR test.
Even if chronic kidney disease seems gradual, these signs can appear suddenly, answering if CKD can happen suddenly.
How Can Early Detection Prevent Sudden Complications?
Emphasis on early detection through comprehensive kidney care helps prevent sudden CKD complications like end-stage renal disease. Catching chronic kidney disease early allows for interventions that slow progression and avoid acute issues. This proactive monitoring addresses concerns about whether chronic kidney disease can happen suddenly.
Early intervention helps manage risk factors such as hypertension, reducing the chance of sudden worsening. For example, a patient with high blood pressure who gets regular checkups can adjust medications promptly. This prevents acute kidney injury and helps preserve kidney function.
-
Get an annual eGFR test to measure kidney filtration rate and spot declines early.
-
Check urine albumin levels to detect protein leakage, a key sign of damage.
-
Consult a nephrologist for personalized comprehensive kidney care plans.
These steps enable patients to act before complications arise. Regular monitoring builds a safety net against sudden events and improves quality of life through timely adjustments.
Who Is at Highest Risk for Rapid CKD Decline?
Individuals with diabetes, hypertension, or kidney stones face rapid CKD decline. These groups often experience sudden worsening of chronic kidney disease due to ongoing damage. Early monitoring helps prevent quick progression.
Diabetics top the list because high glucose levels harm kidney filters over time. This damage can accelerate suddenly under stress. Regular blood sugar checks are key to slowing decline.
Hypertensives follow closely, as high blood pressure strains kidney vessels. Sudden spikes can trigger fast CKD worsening. Controlling pressure through lifestyle changes offers protection.
Schedule a nephrology evaluation for personalized plans to track and manage these risks effectively.
Diabetics and Glucose Damage
Diabetics face the highest risk for rapid CKD decline from prolonged high glucose harming kidney structures. This can happen suddenly during infections or poor control. Can chronic kidney disease happen suddenly? Yes, in uncontrolled cases.
Glucose buildup damages tiny kidney blood vessels, leading to scarring. Patients may notice swelling or fatigue as signs. Daily monitoring of blood sugar helps prevent escalation.
Experts recommend pairing medication with diet adjustments. For example, limit sugary foods and check A1C levels often. This approach supports kidney health long-term.
Hypertensives and Vessel Strain
People with hypertension risk sudden CKD worsening as high pressure damages kidney arteries. Spikes from stress or salt intake can trigger quick decline. Proactive management is essential.
Strained vessels lose flexibility, reducing blood flow to kidneys. Symptoms like high creatinine may appear quickly. Track blood pressure daily at home for early alerts.
Practical steps include low-salt meals and exercise combined with prescribed medications. Regular checkups catch issues before they speed up.
Post-Transplant Patients
Post-transplant patients are prone to rapid CKD decline from immune reactions or drug side effects. Rejection episodes can cause sudden function loss. Close follow-up is critical after surgery.
Medications to prevent rejection often stress kidneys over time. Watch for rising creatinine or fatigue. Adjust doses under medical guidance promptly.
Maintain hydration and avoid over-the-counter painkillers when possible. These habits help protect the transplanted kidney. Consult specialists for tailored monitoring schedules.
Kidney Stone Sufferers
Those with kidney stones risk abrupt CKD progression from blockages or infections. Stones can obstruct urine flow suddenly, harming tissue. Prevention focuses on hydration and diet.
Repeated stones lead to scarring and faster decline. Pain or blood in urine signals trouble. Seek imaging tests during flare-ups.
Drink plenty of water daily and reduce oxalate-rich foods. These changes lower stone formation risk. Early intervention helps prevent rapid damage.
What Role Does a Nephrologist Play in CKD Management?
A nephrologist delivers trusted CKD management with a patient-centric, evidence-based focus. Comprehensive services cover chronic kidney disease, dialysis, and hypertension disorders. Patients benefit from specialized expertise when addressing concerns like whether chronic kidney disease can happen suddenly.
Early intervention helps prevent progression. Care typically spans from initial diagnosis to long-term dialysis support. Clear communication and proven strategies build trust and improve outcomes.
For hypertension linked to CKD, treatments are tailored to control blood pressure and protect kidney function. This holistic care helps patients navigate complexities, including sudden symptom flares. Specialized oversight supports optimal results.
Ongoing monitoring ensures CKD does not escalate unexpectedly. Reliable guidance and structured follow-up improve long-term kidney health.
Expert Diagnosis and Personalized Treatment Plans
Expert diagnosis includes advanced tests for CKD, leading to tailored plans like post-transplant follow-up. This process answers key questions, such as whether chronic kidney disease can happen suddenly, by identifying risks early and enabling prompt action.
A structured approach often follows these steps:
-
Initial assessment: Review symptoms, medical history, and family background to spot patterns.
-
Diagnostics: Order eGFR blood tests and kidney ultrasound for accurate staging.
-
Personalized plan: Combine lifestyle changes, like diet adjustments, with medications to slow progression.
-
Monitoring: Schedule quarterly checks to track improvements and adjust as needed.
Avoid the common mistake of ignoring family history, which can signal genetic risks for sudden CKD worsening. Practical examples include advising low-sodium diets for hypertension control. Evidence-based care improves kidney function stability over time.
Consistent follow-up supports better outcomes. Post-diagnosis plans often incorporate exercise to manage weight and blood sugar, ensuring comprehensive care tailored to individual needs.
Advanced Treatments for CKD in Siliguri
Advanced CKD treatments in Siliguri include hemodialysis, peritoneal dialysis, and kidney stone evaluation. These options help manage chronic kidney disease effectively, even when patients worry whether chronic kidney disease can happen suddenly. Early access to such care helps prevent rapid progression.
For those with advancing CKD, treatments focus on dialysis types suited to lifestyle needs. Hemodialysis fits center-based care, while peritoneal dialysis allows home use. Kidney stone evaluation adds non-invasive checks for related issues.
Patients benefit from local access to these therapies. Treatment plans are tailored based on CKD stage and mobility. This approach supports long-term kidney health amid sudden symptom concerns.
| Treatment |
Type |
Best For |
Program Detail |
Access in Siliguri |
| Hemodialysis |
In-center |
Advanced CKD |
Structured dialysis program |
Available daily sessions |
| Peritoneal dialysis |
Home-based |
Mobile patients |
Home dialysis training |
Home delivery kits |
| Kidney stone evaluation |
Non-invasive |
Stone-related pain |
Imaging and lab assessment |
Local ultrasound access |
| Post-transplant follow-up |
Monitoring |
Transplant patients |
Scheduled function review |
Regular clinic visits |
Top Choice for Stage 4 CKD: Hemodialysis
Hemodialysis stands out as the top choice for Stage 4 CKD. It filters blood effectively when kidneys fail, addressing concerns about sudden deterioration. Sessions last 3–4 hours, typically three times weekly.
In-center hemodialysis provides close monitoring by trained staff. Treatments are adjusted based on fluid balance and lab results. This helps prevent complications from sudden declines.
For Stage 4 patients, it provides critical support before transplant. Practical tips include tracking diet and medications. Siliguri clinics often offer flexible scheduling.
Peritoneal Dialysis for Mobile Lifestyles
Peritoneal dialysis works well for mobile patients needing home-based care. It uses the abdominal lining to filter waste, which can be helpful if CKD progresses unexpectedly. Patients receive training on daily exchanges.
This option fits active routines without frequent center visits. Supplies are delivered at home in Siliguri. Proper hygiene reduces infection risks.
It is often recommended for those who prefer independence. Monitor for signs like abdominal pain and report concerns early. Combining it with dietary changes supports better outcomes.
Lifestyle Guidance to Slow CKD Progression
Lifestyle guidance plays a key role in slowing CKD progression and enhancing outcomes. These steps help manage symptoms and protect kidney function, even if chronic kidney disease appears to worsen suddenly in some cases. Small, consistent changes can make a significant difference over time.
My Husband Has Chronic Kidney Disease: How To Take Care Of Him
Experts recommend focusing on daily habits that support kidney health:
-
Follow a low-sodium diet to control hypertension and reduce kidney strain.
-
Keep blood pressure under 130/80 through medication and healthy habits.
-
Aim for 150 minutes of exercise per week, such as walking or swimming.
-
Maintain hydration balance by drinking adequate fluids without excess.
-
Quit smoking to improve blood flow and slow kidney damage.
Regular check-ups ensure timely adjustments. Research suggests these practices can slow GFR decline and improve overall stability.
Why Low-Sodium Diets Help Control Hypertension
A low-sodium diet reduces fluid retention and lowers blood pressure stress on kidneys. Limit salt intake to under 2,300 mg daily, focusing on fresh foods over processed ones. This supports slower CKD progression.
Read labels carefully and use herbs for flavor. Many patients report reduced swelling and better energy. Combined with other habits, results improve further.
How Does Chronic Kidney Disease Cause Hypertension?
Early dietary changes act as prevention against sudden worsening. Tracking sodium intake with a food diary improves accountability.
Maintaining Blood Pressure Below 130/80
Target blood pressure below 130/80 to protect kidney filters from ongoing damage. Regular home monitoring and follow-up visits guide medication adjustments. This control helps prevent further kidney decline.
Relaxation techniques like deep breathing can complement medication. Weight management also supports this goal. Consistent tracking often leads to measurable improvement.
Vigilance helps guard against sudden CKD flares. Lifestyle adjustments provide steady protection.
Exercise: 150 Minutes Weekly for Kidney Health
Aim for 150 minutes of moderate exercise weekly, such as brisk walking. This improves circulation and supports weight and blood sugar control. Kidneys benefit from improved cardiovascular health.
Break it into 30-minute sessions five days a week. Begin gradually if new to exercise. Pair activity with proper hydration.
Even if CKD progression feels sudden, exercise strengthens resilience. Patients often gain stamina and confidence.
Balancing Hydration Without Overload
Hydration balance means drinking enough to flush toxins without overburdening kidneys. Clear or light-yellow urine is a general guide, though fluid needs vary individually. Follow personalized advice when needed.
Avoid sugary beverages and monitor intake during hot weather. Thirst cues are helpful for many people.
Proper hydration helps reduce risks when chronic kidney disease worsens unexpectedly. It promotes long-term kidney stability.
Quitting Smoking to Preserve Kidney Function
Smoking cessation improves blood vessel health and oxygen delivery to kidneys. Quitting reduces toxin exposure that accelerates kidney damage. Benefits begin within weeks.
Consider support groups, nicotine replacement therapies, or counseling. Replace smoking with healthier routines like walking or hobbies. Tracking progress strengthens motivation and long-term success.

You can reach Dr. Vishal Golay at Remedy Clinics, Singalila Park, Fortune Plaza, Dagapur, Siliguri, or at Balaji Healthcare, 2nd Mile, Sevoke Road, Siliguri by calling 74309 23244 or emailing vishalgolay1980@gmail.com for comprehensive kidney disease and hypertension management.

 7430923244
7430923244